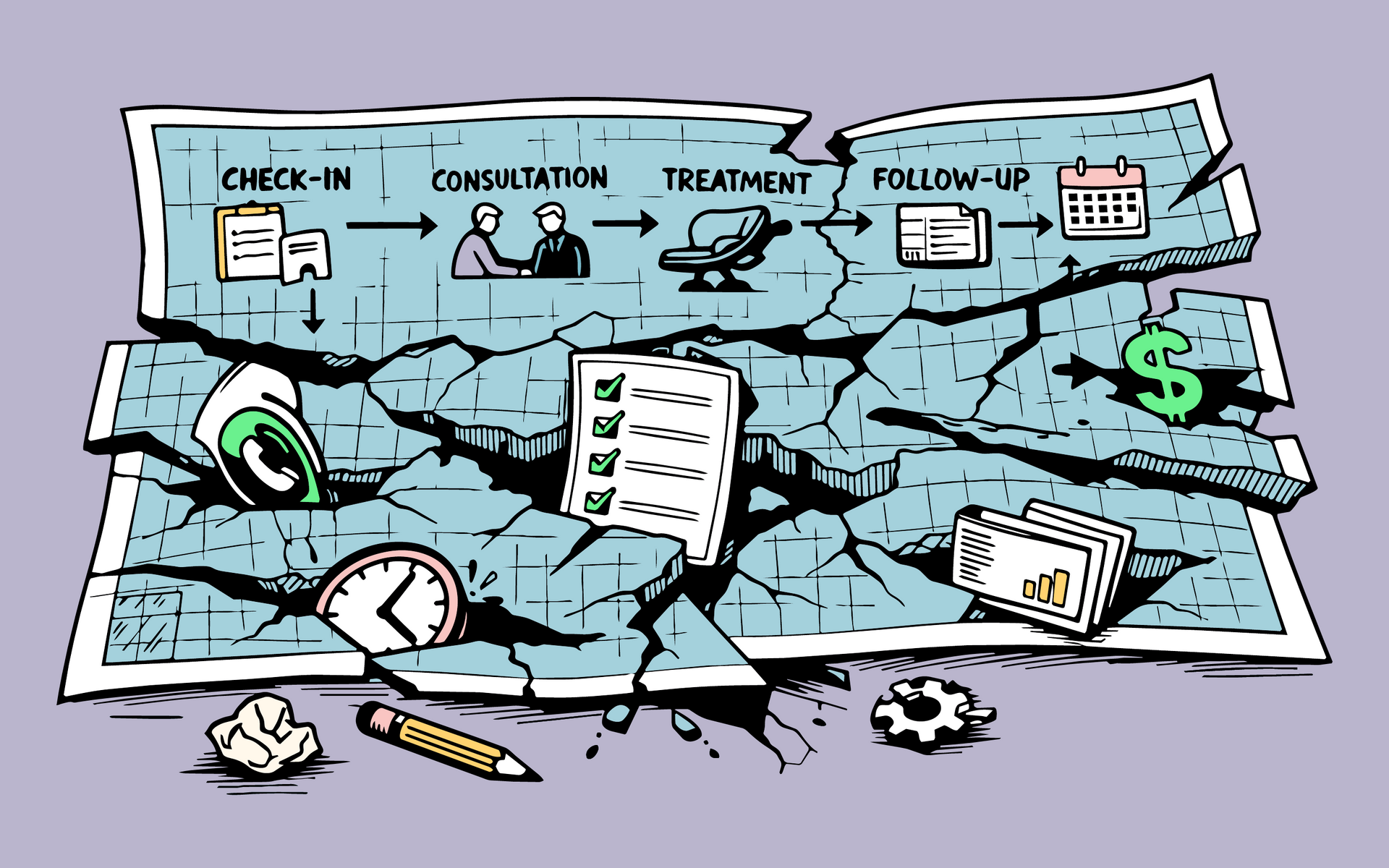
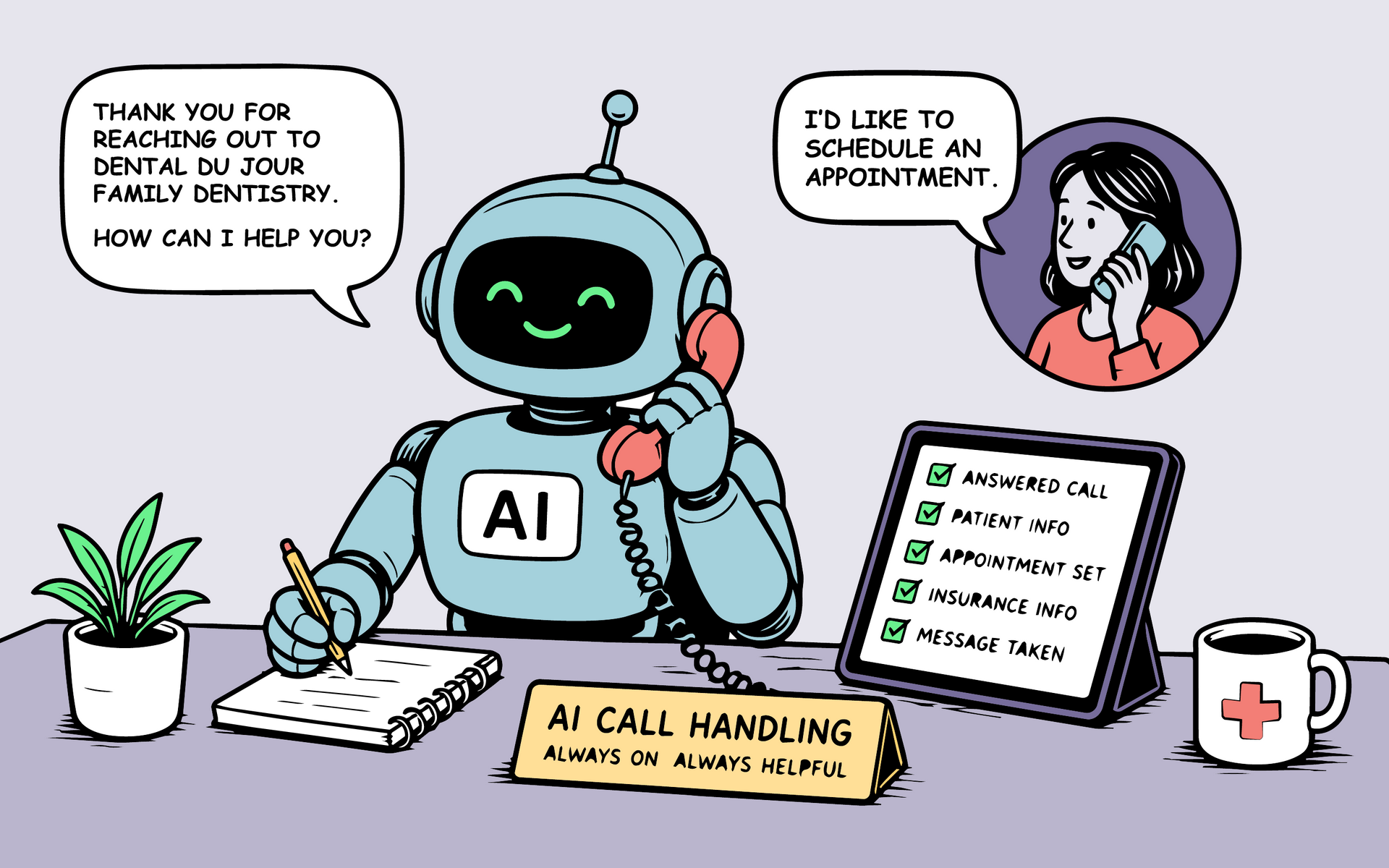
Why Do Most Dental Patient Journeys Fail in Real Life?
By • April 29, 2026

Even When They Look Good on Paper...
The dental industry has spent years perfecting the blueprint. The problem was never the blueprint. It was assuming the blueprint would hld on its own.
Over the last several years, the dental industry has gotten remarkably good at mapping the patient journey. Frameworks exist for every stage, from the first phone call to post-treatment follow-up. Roles are assigned. Metrics are tracked. Best practices are documented and distributed. Walk into most practices today and you will find a team that knows exactly what should happen at every step.
And yet the same problems keep showing up. Missed calls that never get returned. Unscheduled treatment that ages out. Case acceptance that stays stubbornly flat. Follow-through that depends entirely on who is working that day.
Not because practices lack knowledge. Because what is defined on paper does not hold up in practice.
The Assumption That Breaks Down
Most patient journey frameorks rest on a quiet assumption: define the process clearly enough, and the team will execute it consistently. It is a reasonable assumption. It is also wrong.
Dental practices do not operate in controlled environments. They operate in constant variability. Staff turnover, schedule pressure, competing priorities, and simple human inconsistency all chip away at even the best-designed processes. What looks clean in a workflow document becomes fragmented under a full schedule on a Tuesday afternoon.
That fragmentation is where the real leakage begins. Most practices do not have a process problem. They have a consistency problem.
Where the Journey Actually Breaks
The failure point is never the design. It is execution, and it happens quietly across multiple touchpoints at once. A call gets missed and no one loops back. A patient leaves without scheduling the recommended treatment. A follow-up task sits in a queue until it disappears. A financial conversation gets rushed because the schedule is backed up.
Each moment feels minor in isolation. Collectively, they compound into real revenue loss and the kind of operational instability that is hard to diagnose because the practice still feels busy. That is the trap. Activity is not the same as performance. A full schedule is not the same as an efficient one.
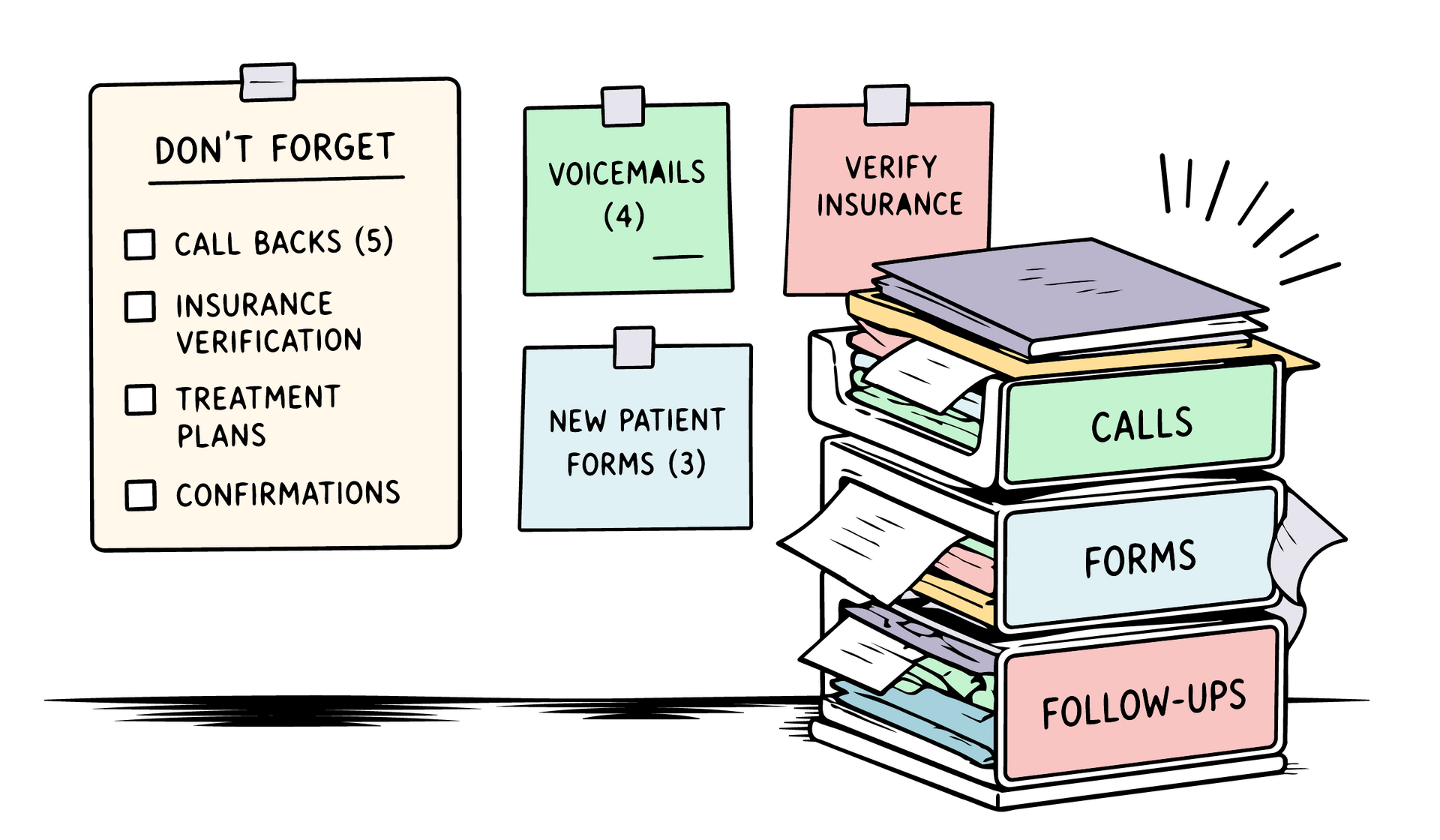
"Busy" does not mean optimized.
"Full" does not mean efficient.
The Illusion of Visibility
Many practices believe they have the situation under control because they track the right metrics: call volume, production, case acceptance, hygiene utilization. But visibility is not the same as control. Knowing how many calls were missed last month tells you what happened. It does not ensure that missed calls get recovered today.
Tracking reveals the past. It does not enforce the future. And that distinction is where most systems quietly fail.
Why Improvements Do Not Stick
The standard response to execution drift is familiar: new scripts, updated SOPs, additional training, another tool in the stack. And those interventions often work, for a while. Then performance slides back. Not because the strategy was wrong, but because nothing is ensuring ongoing adherence once the initial energy fades.
Without that enforcement layer, every improvement depends on memory, motivation, and individual accountability. Those are not stable foundations. They are variables. And under daily pressure, variables lose.
What the Framework Is Missing
The gap is not more detail in the patient journey. Most practices already have plenty of detail. What is missing is stability: a system that ensures processes are not just defined but consistently executed, that tasks are not just assigned but completed, and that performance is not just reviewed occasionally but continuously reinforced.
A well-designed journey that does not hold under real conditions will always produce inconsistent results. And inconsistent results are where revenue disappears.
A Better Question to Be Asking
Instead of asking whether you have the right patient journey, the more useful question is: how much of your patient journey actually holds up day to day? That is a fundamentally different inquiry. It does not measure intent. It measures execution.
When practices start evaluating their operations through that lens, something becomes clear. The issue is not a growth problem. It is a system reliability problem. And until that is addressed, no amount of marketing, training, or new tooling will fully close the gap.
See what SOPHIE AI can do for you!
Apply for the 2-Week Stability Test
You will have a dedicated resource walking you through the process.
This offer is only valid for a short time and space is limited.
SHARE THIS
Latest Posts