The $300K Leak Most Dental Practices Already Know About (But Still Don’t Fix)
Most dental practices don’t have a growth problem.

They have operational leaks...visible, familiar, and quietly costing them hundreds of thousands of dollars every year.
What’s surprising isn’t that these problems exist. It’s that they continue, even after being identified, discussed, and measured.
The issue isn’t awareness. It’s execution that doesn’t hold.
The Industry Already Knows Where the Problems Are
Spend a few minutes in any dental Facebook group or forum, and you’ll see the same patterns repeated over and over. Practice owners, consultants, and coaches are all pointing to the same issues: missed calls, underperforming hygiene, low case acceptance, operational bottlenecks.
This isn’t hidden. It’s not emerging insight. It’s widely understood across the industry.
Here’s a recent example that circulated in one of those groups:
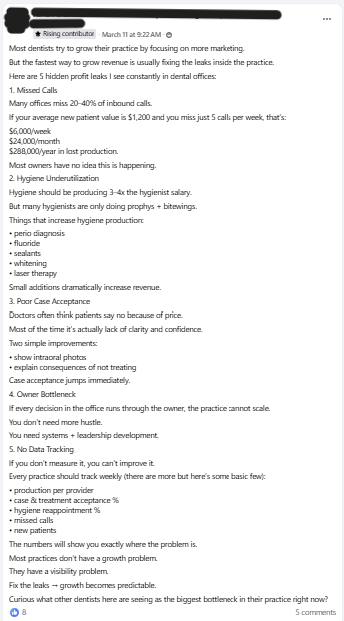
Everything in that breakdown is accurate.
The math is real. The observations are valid. The recommendations are reasonable.
And yet...these same problems continue to show up in the same practices, month after month, year after year.
So the real question isn’t where the leaks are. It’s why they persist even after they’re clearly identified.
The problem isn’t finding the leaks.
It’s that they keep coming back.
The $300K Leak Hiding in Plain Sight
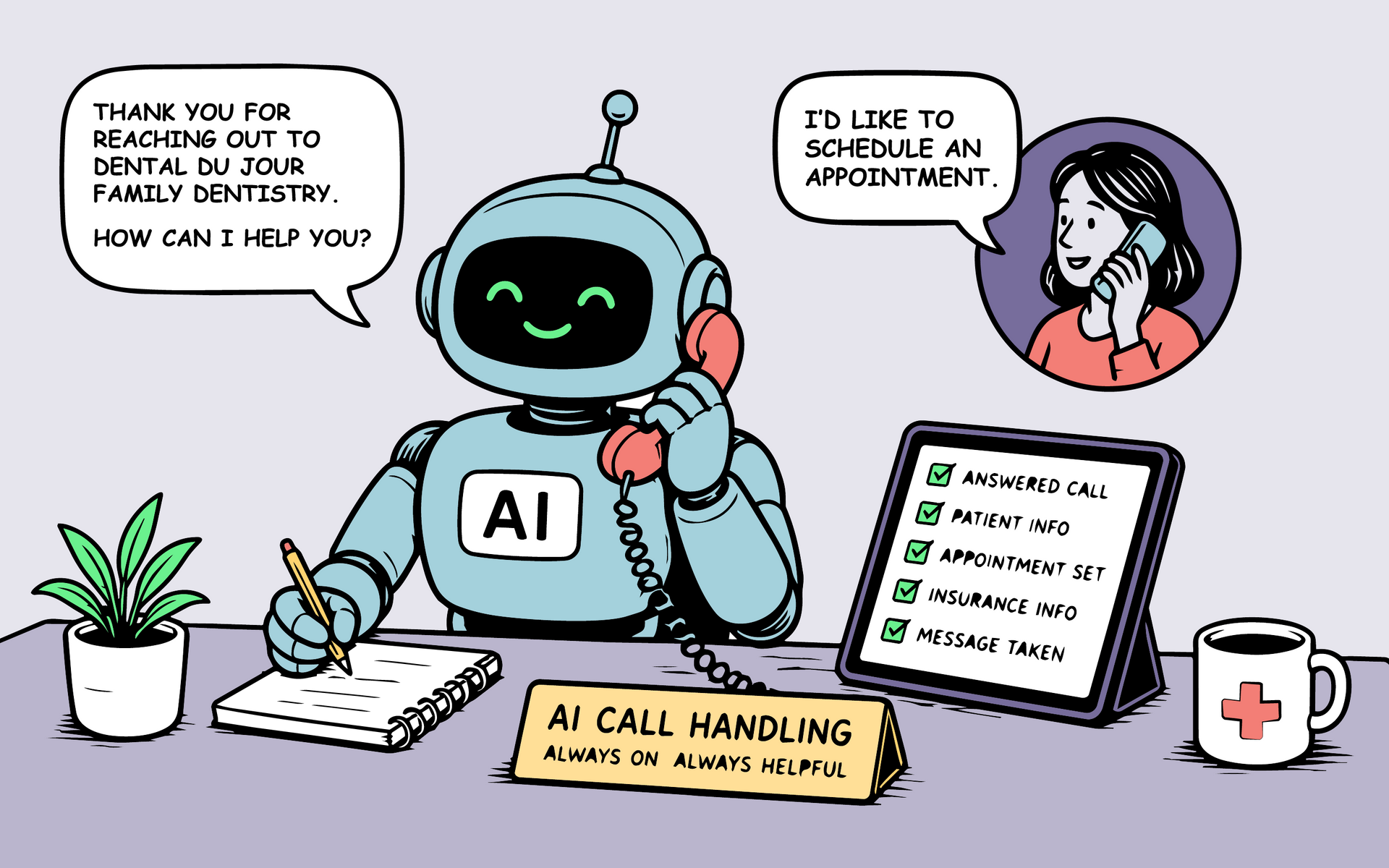
Take just one of the examples from that post: missed calls.
If a practice misses five new patient calls per week, and the average new patient value is $1,200, that translates to $6,000 per week in lost production. Over the course of a month, that becomes $24,000. Over a year, it approaches $288,000 in missed opportunity.
A single leak (like missed calls) can compound quickly:
- 5 missed calls/week
- $1,200 avg patient value
- ≈ $288,000/year lost
And that’s only one category.
When you layer in unscheduled treatment, recall breakdowns, inconsistent case presentation, and delays in insurance follow-up, the total impact compounds quickly. Most practices are not losing small amounts here and there. They are leaking a meaningful percentage of total production.
In many cases, that number falls between ten and twenty percent annually.
What makes this more frustrating is that none of these leaks are unknown. Most practices can point to them immediately. Many are already tracking them in reports or discussing them in meetings.
Which raises an uncomfortable reality: Knowing where money is being lost does not mean it will be recovered.
Knowing where money is being lost does not mean it will be recovered.
Most practices aren’t missing opportunities.
They’re leaking revenue they’ve already earned.
Why Visibility Doesn’t Fix the Problem
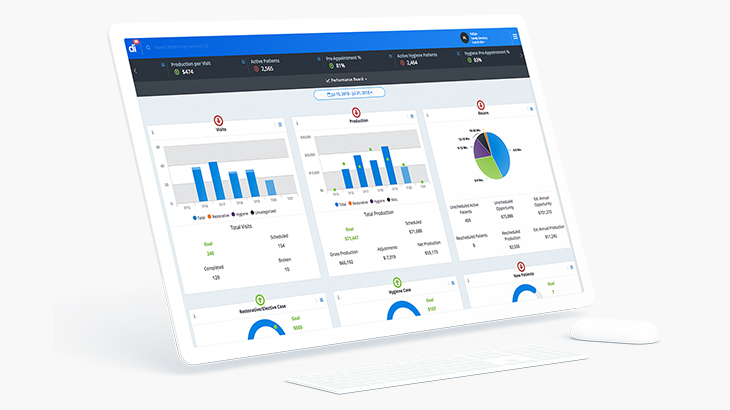
There is no shortage of visibility in modern dental practices.
Offices have dashboards, reporting tools, consultants, and regular meetings. They review numbers, set goals, and talk through opportunities for improvement. On paper, it appears that everything needed to improve performance is already in place.
But visibility operates in hindsight. It tells you what happened, not what is actually being carried out in real time.
That gap becomes obvious in the day-to-day reality of a practice. A morning huddle sets clear priorities, but by mid-afternoon the schedule has shifted, interruptions have piled up, and the original plan has drifted. A system for returning missed calls exists, but when the front desk gets overwhelmed, it stops being followed. Case presentation protocols are defined, but vary depending on who is delivering them and how busy the day feels.
The problem isn’t that these systems don’t exist.
It’s that they don’t hold under pressure.
You don’t have a visibility problem.
You have a stability problem.
What Actually Breaks Inside the Practice
When you look closely, every one of these “known” problems shares the same underlying failure point. They depend on consistent execution in an environment that is constantly changing.
A practice doesn’t break because it lacks ideas or strategies. It breaks because execution becomes inconsistent when conditions are less than ideal...when the schedule gets tight, when staff changes, when priorities compete, or when no one is directly accountable in the moment.
This is why practices can implement training, install new tools, document SOPs, and still see the same issues persist. The structure exists, but it isn’t reinforced in a way that ensures it is followed.
That’s the difference between something that is designed to work and something that actually works.

It’s not what your systems say.
It’s what your team actually does when the day gets busy.
The Problem Isn’t Visibility. It’s Stability.
The industry continues to frame this as a visibility problem. Track more metrics. Review performance more often. Add better reporting.
But visibility alone does not create consistency. The real constraint is whether the practice has a system that ensures what should happen actually happens...consistently, across people, across roles, and across days.
Without that, everything becomes dependent on effort, memory, and individual discipline. And those are inherently unreliable under pressure.
This is why the same leaks keep reappearing, even in practices that are actively trying to fix them.
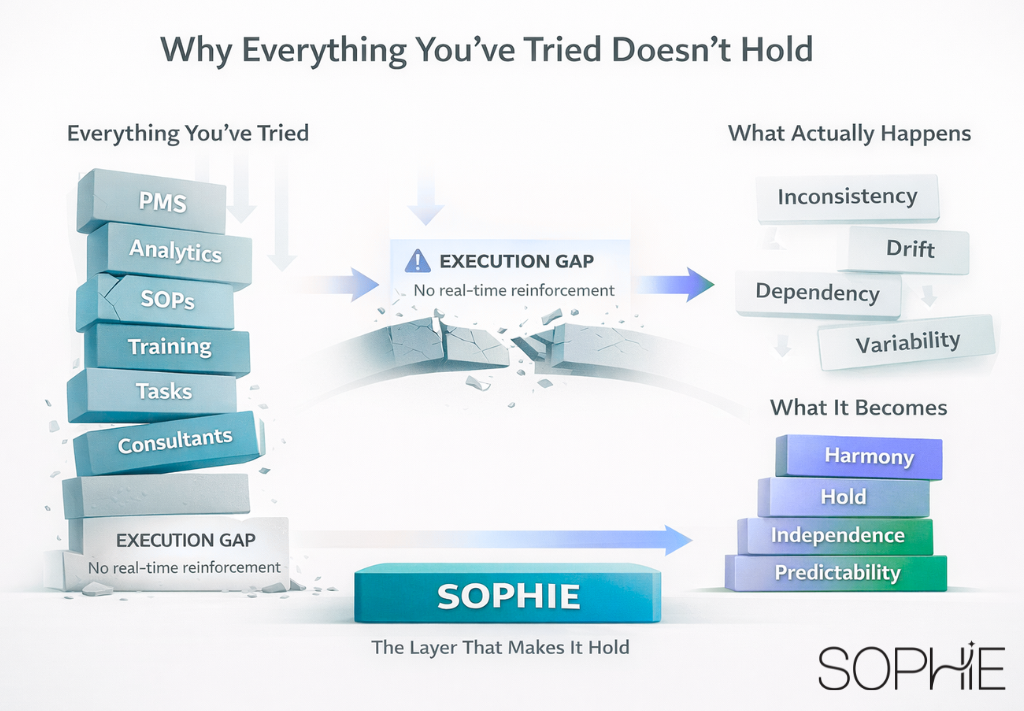
The Stability Layer Most Practices Are Missing
Every operational area mentioned in that original breakdown—missed calls, hygiene production, case acceptance, follow-up—relies on a set of conditions that most practices don’t fully have in place.
They require standards that are not only defined, but enforced. They require visibility that doesn’t just report issues, but surfaces them in time to act. They require accountability that is embedded into the workflow, not dependent on reminders or meetings.
Without that layer, improvements remain temporary. They work when attention is high and conditions are controlled, but fade as soon as the environment becomes more complex.
This creates the illusion of progress without sustained change.

Measuring What Actually Holds
If the problem isn’t identifying leaks, but ensuring execution holds, then the question changes.
Instead of asking, “Where are we losing money?” the more useful question becomes:
How much of what we already know is actually being executed consistently?
This is the foundation behind the SOPHIE Practice Stability Assessment.
Rather than focusing on isolated metrics, the assessment evaluates how reliably the practice operates across five core areas:
- revenue capture
- patient flow and scheduling
- financial workflow discipline
- team execution
- operational governance
From that, it produces a Practice Stability Score, an Operational Risk Index, and a modeled estimate of how much revenue is currently exposed due to inconsistency.
For example, a practice generating $3 million annually with a mid-range stability score may be losing roughly twelve percent of its production to operational leakage. That equates to approximately $360,000 in annual revenue exposure, with a significant portion of that recoverable through improved execution.
This reframes the problem in a way that most practices haven’t quantified before.
It’s not just that leaks exist.
It’s how much of the business depends on systems that don’t consistently hold.
| Area | What Practices (Should) Track | What Actually Fails |
|---|---|---|
| Revenue Capture | Case acceptance % | Follow-up consistency |
| Patient Flow | Schedule utilization | Follow-up consistency |
| Financial Workflows | AR reports | Missed call recovery |
| Team Execution | SOP documentation | Execution discipline |
| Operational Governance | SOP documentation | Adherence under pressure |
The Shift That Actually Drives Growth
Most practices try to grow by adding more...more marketing, more staff, more tools. But growth rarely comes from adding complexity to an unstable system. It comes from stabilizing what already exists.
When execution becomes consistent, missed calls get returned, treatment gets scheduled, patients follow through, and workflows don’t break when the day gets busy.
At that point, growth becomes far more predictable. Not because new strategies were introduced, but because existing ones finally hold.
How Much of Your Practice Actually Holds Under Pressure?
Most practices already know where they’re losing money. What they don’t know is how much of that loss is driven by inconsistency, or how much is realistically recoverable.
The SOPHIE Practice Stability Assessment is designed to answer that. It gives you a clear view of your stability score, your operational risk, your estimated revenue exposure, and the specific areas where execution is breaking down.
From there, the path forward becomes far more concrete.
Not another idea to implement.
But a system to ensure what matters actually happens.
If it doesn’t hold under pressure, it’s not a system.