Why Most Dental Patient Journeys Fail in Real Life (Even When They Look Perfect on Paper)
The Industry Has Already Solved the “What”

Over the last few years, the dental industry has gotten significantly better at defining the patient journey. There are frameworks mapping every stage...from the first phone call to follow-up care. Roles are assigned. Metrics are identified. Best practices are documented.
On paper, it’s all there:
- Calls should convert
- Patients should feel welcomed
- Diagnoses should be clear
- Treatment should be accepted
- Follow-ups should be consistent
And yet, despite all of this clarity, most practices are still experiencing the same problems:
Missed calls.
Unscheduled treatment.
Declining case acceptance.
Inconsistent follow-through.
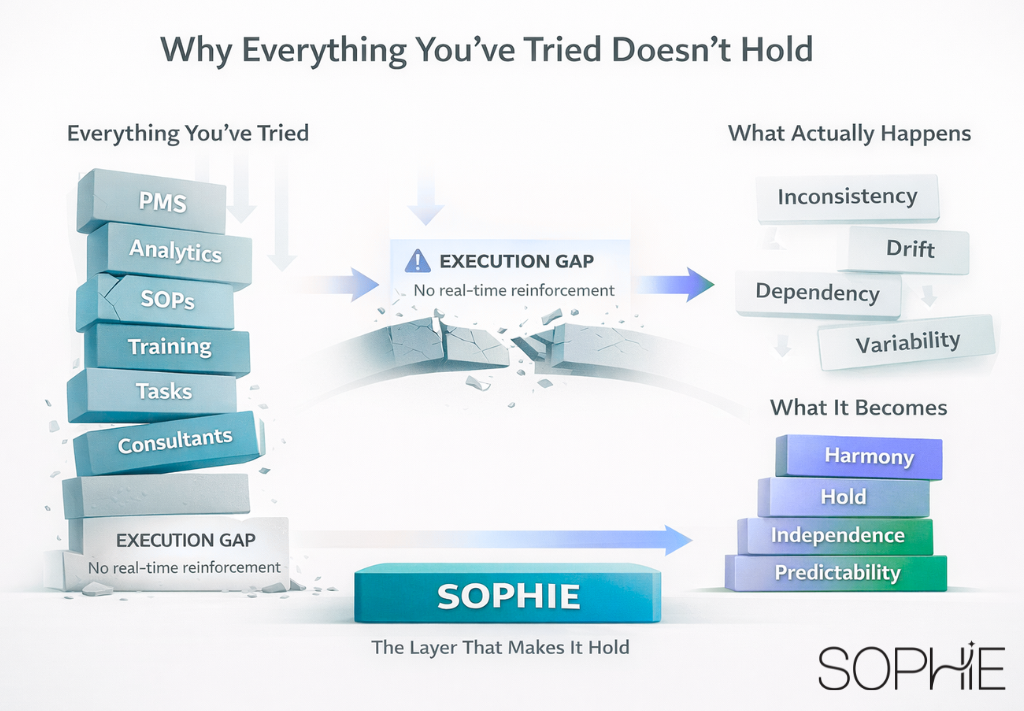
Not because they don’t know what to do. Because what’s defined… doesn’t hold.
The Gap No One Talks About
The assumption behind most patient journey frameworks is simple:
If you define the process clearly enough, the team will execute it consistently.
That assumption breaks down in real life.
Because dental practices don’t operate in controlled environments. They operate in constant variability:
- Staff turnover
- Busy schedules
- Interruptions
- Competing priorities
- Human inconsistency
What looks clean and structured in a blueprint becomes fragmented under pressure.
And that’s where the real leakage begins.
Most practices don’t have a process problem.
They have a consistency problem.
Where the Patient Journey Actually Fails
It doesn’t fail in the design. It fails in execution...quietly, repeatedly, and across multiple points in the system.
A call gets missed and never returned.
A patient leaves without scheduling treatment.
A follow-up task is assigned but never completed.
A financial conversation is rushed or avoided.
Each moment feels small. But collectively, they compound into significant revenue loss and operational instability.
This is why a practice can feel “busy” while still underperforming. Because activity is happening. But execution isn’t holding.

Busy does not mean optimized.
Full does not mean efficient.
The Illusion of Visibility
Many practices believe they have control because they track metrics:
- Call volume
- Production
- Case acceptance
- Hygiene utilization
But visibility is not the same as control.
You can know:
- how many calls were missed
- what your case acceptance rate is
- how full your schedule looks
And still have no system ensuring that:
- missed calls are recovered
- follow-ups are executed
- treatment plans are consistently reinforced
Tracking reveals what happened. It does not enforce what should happen next.
Why Improvements Don’t Stick
This is where most practices (and most consultants) get stuck.
They introduce:
- new scripts
- new SOPs
- new training
- new tools
And for a short period, things improve. Then performance regresses. Not because the strategy was wrong. But because there is no system ensuring ongoing adherence.
Without that layer, every improvement depends on:
- memory
- motivation
- individual accountability
And those are inherently unstable.
If you rely on people remembering what to do, that "system" will eventually break.
The Missing Layer: Stability
What’s missing from most patient journey frameworks isn’t more detail.
It’s stability.
A stable practice is one where:
- processes are not just defined, but consistently executed
- tasks are not just assigned, but completed
- performance is not just reviewed occasionally, but continuously reinforced
This is the difference between:
- knowing what should happen
- and ensuring it actually does
From Journey to Reality
The patient journey is still valuable. It provides structure. It creates alignment. It defines expectations.
But on its own, it is incomplete.
Because a well-designed journey that doesn’t hold under real conditions will always produce inconsistent results.
A Better Question to Ask
Instead of asking:
“Do we have the right patient journey?”
Practices should be asking:
“How much of our patient journey actually holds up day to day?”
That’s a very different question. Because it doesn’t measure intent. It measures execution.
Where This Leads
When practices begin to evaluate their operations through this lens, something becomes clear:
They don’t have a growth problem.
They have a system reliability problem.
And until that is addressed, no amount of marketing, training, or tooling will fully close the gap.
If you want to understand how much of your current system is actually holding—and where it’s breaking—you can start by measuring it.
The Practice Stability Assessment evaluates:
- where execution is inconsistent
- where revenue is leaking
- and how much of that is recoverable
Because before you try to grow, you need to know what’s already slipping through.